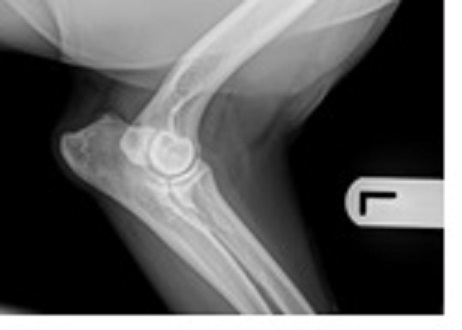
Elbow dysplasia (ED) is one of the most common causes of thoracic limb lameness in Labradors and other large- and giant-breed dogs (Michelsen, 2013). ED is a term used to describe the presence of one or more developmental conditions that involve the elbow joint.
This collective term includes conditions such as medial coronoid disease (MCD), radio-ulnar incongruity, ununited anconeal process (UAP) and osteochondrosis (OCD) (Cook and Cook, 2009; Kirberger and Fourie, 1998; Michelsen, 2013; Samoy et al., 2006). These conditions develop in juvenile animals and clinical signs (pain and lameness) are often present at four to six months of age. However, many dogs do not present until much later, when their osteoarthritis (OA) is advanced and lameness is a constant feature.
Current treatment and management for elbow dysplasia
There have been many techniques for both medical and surgical management for ED described in the literature (Fitzpatrick et al., 2013, 2015; Fitzpatrick and Yeadon, 2009; Gutbrod and Guerrero, 2012; McConkey et al., 2016; Michelsen, 2013; Quinn and Preston, 2014; Samoy et al., 2013):
- Arthroscopic treatment
- Ulnar osteotomies
- Proximal ulnar osteotomy
- Distal ulnar osteotomy
- Biceps ulnar release procedure
- Proximal abducting ulnar osteotomy
- Sliding humeral osteotomy
- Canine uni-compartment elbow replacement
- Full elbow replacement
- Elbow arthrodesis
However, irrespective of which medical or surgical intervention is performed, ED leads to cartilage damage and degenerative OA with time (Burton et al., 2011; Dempsey et al., 2019). The only exception to this would be full elbow replacement, but this procedure is not currently recommended due to the high complication rate.
OA leads to a progressive degenerative state in the joint that inevitably leads to chronic pain and loss of limb function. The number of surgical procedures described in the literature shows that no one technique is 100 percent effective, and the multifactorial causes of ED provide challenges to effective surgical treatment.
Irrespective of which medical or surgical intervention is performed, elbow dysplasia leads to cartilage damage and degenerative osteoarthritis with time
In cases of ED, arthroscopy is commonly performed to aid diagnosis, perform fragmented coronoid process (FCP) removal and remove diseased cartilage. This leads to potential short-term benefits in improved function and pain reduction; however, the long-term prognosis has been shown to be no different to conservative management (Burton et al., 2011; Dempsey et al., 2019).
Conservative management involves analgesic medications, exercise restriction, environmental adaptation and maintaining an ideal body condition score. In addition, physical therapies can form part of a conservative approach through modalities such as physiotherapy and hydrotherapy. However, conservatively managed patients will also go on to develop OA eventually, and these cases can be difficult to manage effectively.
More recently, a variety of intra-articular treatments have been trialled and have shown some promise in managing ED conditions using a multimodal approach. Hyaluronic acid and other joint lubricants have been used to help smooth joint articulation in OA, but medium- to long-term effects appear to be limited.
Innovations in treatment for elbow dysplasia
The lack of efficacious treatments for ED has resulted in trials of biological therapies such as stem cell therapy and platelet-rich plasma (PRP) (Huňáková et al., 2020; Kim et al., 2019; Kriston-Pál et al., 2017, 2020; Olsen et al., 2019). These therapies, used under a new branch of medicine termed “regenerative medicine” (RM), show great promise in better treating the disease. Furthermore, they have a disease-modifying effect rather than just treating the symptoms such as pain.
Stem cell therapy to treat elbow dysplasia
Greenside Veterinary Practice has been using stem cell therapy, along with PRP, to treat ED for a number of years and has modified its protocols with experience to develop a minimally invasive, highly effective treatment option. Using RM, Greenside is able to stop the degenerative process, reverse some signs of OA and restore joint health.
Although regenerative medicine cannot reverse the disease process [...] Greenside has shown it to be highly effective in managing the condition
Although RM cannot reverse the disease process (the dysplasia or abnormal development of the elbow joint) which results in the formation of OA, Greenside has shown it to be highly effective in managing the condition with outcomes and longevity of effects that outperform many surgical interventions and conservative management (Armitage et al., 2018; Armitage and Reid, 2019).
This treatment allows Greenside to resolve lameness, reduce pain and improve function for extended periods of time. Positive treatment responses commonly last for 18 months to 2 years before a top-up injection is required. However, because RM cannot reverse the underlying ED, with time the joint will start to degenerate again. At this point, further treatment can be provided to regain control and arrest the degenerative process.
Once stem cells have been harvested from the patient by a small surgical procedure under general anaesthetic, the stem cells are cultured to provide the required numbers needed for effective treatment. The stem cells can be stored in liquid nitrogen in a process called cryopreservation, which means practices can have a supply of stem cells usually for the lifetime of the patient. When further treatment is required, practitioners can simply “wake the cells up” at a lab and culture more without having to harvest more adipose tissue (fat) from the patient.
Stem cells can be stored in liquid nitrogen in a process called cryopreservation, which means practices can have a supply of stem cells usually for the lifetime of the patient
Culturing the stem cells has many advantages, such as knowing the exact concentration and viability of cells to provide a reliable “dose” specific to the condition being treated. The sterility, morphology and purity of the resultant cultured stem cells are checked before shipment from the lab to ensure patient safety and ensure the best possible cells are used.
What has Greenside discovered about elbow dysplasia?
Complications from arthroscopic intervention
From the extensive experience of treating ED, Greenside has found that dogs that have undergone arthroscopic intervention before treatment with RM tend to do less well than dogs that have not undergone the procedure.
Practitioners at Greenside believe that this is due to the invasive nature of arthroscopy and the potential to cause further instability and more severe OA changes following FCP removal and curetting of the cartilage. For this reason, they do not advocate the use of arthroscopy to manage ED. Patients that have had arthroscopy need to be treated with RM more aggressively, requiring two treatments 12 weeks apart and the addition of hyaluronic acid into the treatment plan. Greenside has improved its outcomes in these patients, but repeat treatments are more commonly required on an annual basis.
Correlated issues in the shoulders
In patients presenting with ED and OA, the team at Greenside commonly find other problems associated with the disease process in the shoulders. Patients with ED have altered gait and loading patterns due to pain in the medial compartment of the elbow. This results in changes to the directional forces in the shoulder support structures and the tendons involved in shoulder and elbow movement. For this reason, the team always evaluates a patient’s shoulder soft tissue structures with musculoskeletal ultrasound when they present with ED. In the experience of the Greenside team, 95 percent of dogs with ED have concurrent shoulder tendon problems, which can result in another significant source of pain and loss of function.
In addition to the mechanical effects of altered gait, elbows that have advanced OA changes commonly have a significant reduction in range of motion (ROM). This is due to new arthritic bone formation throughout the joint and thickening and fibrosis of the joint capsule, physically obstructing joint flexion and extension. This, in turn, has secondary consequences that result in shoulder tendon degeneration. Disease or degeneration in other parts of the body or other limbs can also play a role due to compensatory adaptations to lameness and pain.
Regenerative medicine is highly effective if used with specific bespoke protocols in treating osteoarthritis and other degenerative conditions such as tendon degeneration
Fortunately, RM is highly effective if used with specific bespoke protocols in treating OA and other degenerative conditions such as tendon degeneration. Not all stem cell treatments and PRP therapies are the same and many have not been validated in dogs which can result in suboptimal treatment outcomes.
Final thoughts
At Greenside, the team has investigated and trialled many different products and believe they have found and validated the best possible products to ensure successful and consistent positive treatment outcomes.
RM is a targeted treatment that requires a holistic approach to treat all causes of pain and degeneration in the body simultaneously to get the best treatment responses. Greenside, therefore, perform a thorough physical examination and further diagnostic tests (X-rays and musculoskeletal ultrasound) to diagnose concurrent orthopaedic musculoskeletal conditions. All musculoskeletal diseases are amenable for treatment using RM if correctly diagnosed and specifically targeted – this includes many spinal conditions. Bloods are also taken to look at the patient’s general health profile and check thyroid levels, as other non-orthopaedic disease processes can affect treatment outcomes if not identified.
Greenside Regenerative Therapies and Rehabilitation was the first specialist referral centre in the UK to provide treatments using stem cell therapy and rehabilitation. It uses objective data to ensure patients are improving and to modify treatments using an evidence-based approach rather than only subjective assessment. After treatment, Greenside monitors patients and provides further support, including home exercise plans and rehabilitative therapies, and offers regular reassessments and remote support as required.
There is no cure for canine elbow dysplasia, but Greenside has developed a more efficacious treatment option providing reduced pain, increased function and a better quality of life for dogs with elbow dysplasia and related issues.
| To find out more about the pioneering regenerative medicine treatment being carried out at Greenside, visit www.stemcellsscotland.co.uk. |